
Avoid Being Caught Unawares by Glaucoma
Early Detection is Key to Getting Prompt Treatment and Preventing Vision Loss
What is Glaucoma?
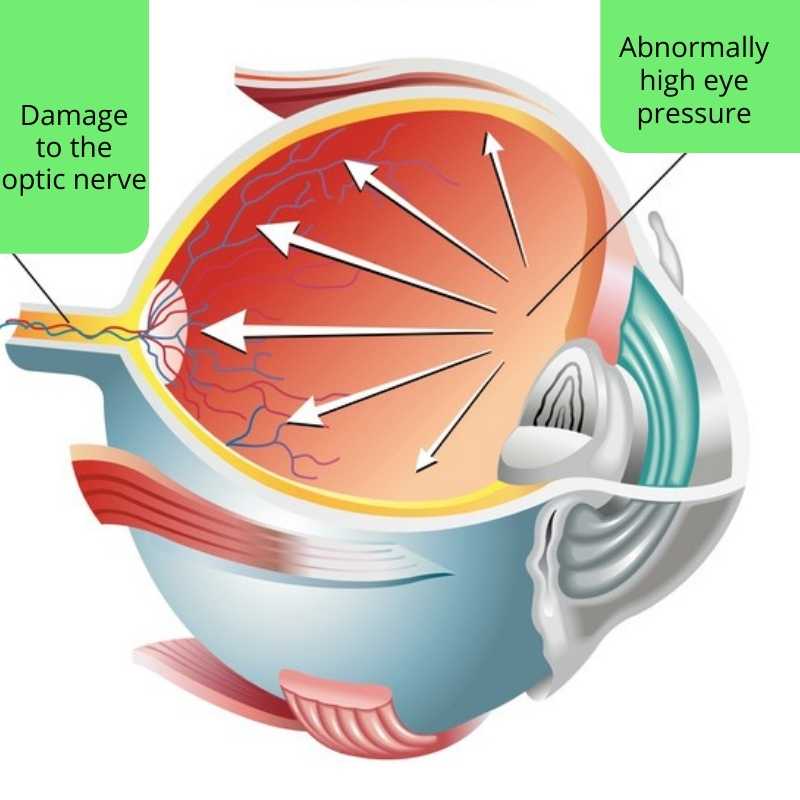
Glaucoma is a group of eye diseases that progressively damage the optic nerve, the part of the eye that transmits visual information from the retina to the brain for interpretation. It is a common eye condition that can lead to vision loss if not detected early and treated properly.
Most people who have glaucoma do not experience symptoms. So, they are usually not aware that they have the disease until they begin to lose their vision. Loss of vision in glaucoma starts from the sides where it is often not obvious. It eventually gets to the centre of one’s vision if it is not treated. Hence, glaucoma is often referred to as the ‘Silent Thief of Sight’.
While glaucoma is treatable, it is currently not curable. Available treatments help prevent the disease from getting worse but they do not cure it. Therefore, any optic nerve damage and vision loss that occurs before starting treatment cannot be recovered.
This is why checking your eyes regularly (every one or two years) is important, particularly if you are at a high risk of developing the disease.
Types of Glaucoma
Glaucoma can be broadly classified into primary glaucoma and secondary glaucoma depending on whether it is caused by another eye condition or not. Primary glaucoma is glaucoma that is not caused by other eye conditions while secondary glaucoma is glaucoma that occurs as a result of other eye conditions.
The major types of glaucoma are open-angle glaucoma, closed angle glaucoma, and normal or low tension glaucoma.
Open-angle glaucoma
This is glaucoma that occurs when the angle between the iris and cornea (filtration angle) through while aqueous humour drains from the eye is open. It is the most common type of glaucoma. The build-up of fluids in the eye despite an open-angle is thought to be due to some abnormalities that cause the drainage channels to gradually get clogged; thereby, reducing the outflow of aqueous humour.
Open-angle glaucoma is a chronic condition and the risk of developing it increases with age. This type of glaucoma affects blacks more and rarely causes symptoms at the early stages.
Closed-angle glaucoma
This is a type of glaucoma caused by narrowing or blockage of the angle through which aqueous humour drains from the eye. It causes a sudden rise in intraocular pressure and can quickly damage the optic nerve. It is more common in Asians and usually has noticeable signs and symptoms such as headaches, severe pain, cloudy and reduced vision, red eyes, nausea/vomiting, halos, and stone-hard eyeballs. Closed-angle glaucoma requires immediate treatment to prevent vision loss
Normal or low tension glaucoma
This is glaucoma that occurs in the presence of normal or low eye pressures. It is believed to be caused by the poor blood supply to the optic nerve or by an unusually pressure-sensitive optic nerve.
Other types of glaucoma
Other types of glaucoma are less common. They include:
- Congenital glaucoma – This is a type of glaucoma that occurs in children. It is inherited and present at birth. It occurs due to a defect in the structures responsible for the drainage of fluid in the eye.
- Neo-vascular glaucoma: This is secondary glaucoma that occurs due to the development of blood vessels in the iris and the clogging of the drainage channels by these blood vessels; thereby obstructing the outflow of aqueous humour. Neovascular glaucoma is usually seen in diabetic patients and patients with ischaemic conditions (conditions that restrict blood supply to tissues). Treatment is targeted at stopping the new vessels from growing and controlling pressure with eye drops.
- Pigmentary glaucoma: This is a rare type of glaucoma that occurs in people with pigment dispersion syndrome, a condition in which granules of pigments fall off the iris and float around in the aqueous humour. The pigment floating in the aqueous humour accumulates over time and eventually blocks the filtration angle increasing the intraocular pressure.
Causes of Glaucoma
The major causes of glaucoma are
- High eye pressure
- Unusually sensitive optic nerve
- Reduced blood flow to the eye.
Any condition that leads to the above-mentioned causes, can also trigger or worsen cause glaucoma.
Increased eye pressure
Increased eye pressure occurs due to the accumulation of aqueous humour in the eye. Aqueous humour is a thin transparent fluid that nourishes the lens and cornea and helps the eye maintain its shape. It accumulates in the eye when there is an imbalance between its production and drainage from the eye. This imbalance can be due to the over-production of the fluid or blockage of the drainage channel. If the high pressure is sustained, it can damage the optic nerve resulting in glaucoma.
Unusually sensitive optic nerve
Glaucoma can also occur under normal eye pressure which ranges from 10 to 21 mm Hg. This is known as normal-tension glaucoma. People who develop glaucoma under this condition are thought to have an unusually sensitive or fragile optic nerve that is susceptible to damage by relatively normal levels of eye pressure.
Reduced blood flow to the optic nerve
When blood flow to the eye is reduced, oxygen supply to the optic nerve becomes inadequate and its nerve fibres gradually die resulting in glaucoma. Glaucoma in this case is often associated with vascular-related disorders such as low blood pressure, migraine headaches, and other diseases that cause poor blood circulation.
Symptoms
Most cases of glaucoma do not show symptoms early. The usual symptom which is observed when the disease has advanced is the loss of side vision.
Few cases of glaucoma may observe the following symptoms:
- Red eye
- Eye pain
- Headache
- Seeing halos around light
- Cloudy vision
Risk Factors for Developing Glaucoma
Anyone can develop glaucoma, however, some people have characteristics and exposures that put them at a higher risk of getting the disease.
Some factors that increase one’s risk of developing the disease include:
- A family history of glaucoma: This is one of the most important risk factors. Glaucoma is hereditary. If a family member, living or dead, has or had the disease, you have a higher risk of developing it compared to someone who does not have a family history of the disease.
- Age: Glaucoma can occur in all age groups but the condition is more common in people aged 40 years and above.
- History of high intraocular pressure: People who have high intraocular pressure are at a higher risk of progressing to glaucoma compared to others with lower eye pressures.
- Having a thin cornea: People whose corneal thickness is thin are at a higher risk of developing glaucoma as pressure measurements may be underestimated.
- Being an African: Blacks have a higher risk of developing glaucoma, particularly the open-angle type. Closed-angle glaucoma is more common in Asians.
- Have/had eye surgery or injury: Having an eye surgery or injury increases the risk of developing glaucoma because of the inflammation that occurs after the surgery or injury.
- Having chronic health conditions such as diabetes, hypertension, heart disease, and sickle cell disease.
- Having high myopia: People who have myopia or short-sightedness are at a higher risk of developing glaucoma.
- Long-term use of steroid medications: Using steroids for a long time (more than 8 weeks) increases the risk of developing glaucoma.
Preventing Glaucoma
How to Prevent Glaucoma
Prevention of glaucoma is not 100% guaranteed, but you can reduce the risk of getting it with a proactive eye care routine. If you already have glaucoma, you can also minimize your risk of vision loss with an eye care routine developed with recommendations from your eye doctor.
The essence of having a routine that you follow is to ensure that your eye pressure level is always normal and that you avoid situations that negatively affect the optic nerve’s supply of oxygen and nutrients.
A good routine will include the following:
1-Eye Protection
The inflammatory response and healing process of eye injuries that can increase eye pressure and lead to glaucoma soon after the injuries or over time if they are not managed properly. By protecting your eyes against hazards, you can prevent eye injuries and minimize your risk of glaucoma.
2-Exercise
Aerobic exercises done safely (moderately) can lower eye pressure and supply the eyes with nutrients and oxygen necessary for a healthy optic nerve. They also helps control chronic health conditions that can cause glaucoma, e.g diabetes. To minimize your risk of glaucoma, perform moderate aerobic exercises like brisk walking, dancing and swimming at least 30 minutes 5 day week.
3-Regular eye check and treatment of glaucoma risk factors
Glaucoma often develops gradually without warning signs. Hence, many people who have it are often not aware until vision loss begins to occur. Regular eye checks (at least once a year) can detect clinical signs of glaucoma like high eye pressure. This gives you a chance to treat it early and prevent it from progressing to glaucoma.
Also, get eye injuries and persistent eye symptoms checked and treated promptly even if you are up to date with your annual check. This is important because eye injuries can lead to the development of glaucoma even many years after the injury occurred.
Diagnosing Glaucoma
Diagnosing glaucoma starts with a glaucoma screening that is either done independently or as part of a comprehensive eye examination at the clinic.

Get Screened For Glaucoma
Glaucoma screening starts with checking the pressure in the eye (intraocular pressure) with an instrument called a tonometer.
The screening also involves assessing how well you can see (visual acuity test), pupils, anterior chamber and optic nerve at the back of the eye.
To get screened, visit our eye clinic during work hours.
If glaucoma is suspected after the screening test, additional tests will be required to confirm or rule out the condition.
Generally the following tests are required for a conclusive diagnosis:
1-Eye pressure test
This is known as tonometry. The normal eye pressure range is 10-21mmHg. Eye pressure above this range is high and a major risk factor for glaucoma. However, since there are cases of glaucoma under normal eye pressure (normal-tension glaucoma), an eye pressure test alone is not enough to diagnose glaucoma.
2-Ophthalmoscopy
This test is done to examine the health of the optic nerve and surrounding retina. If the eye doctor observes abnormalities in the shape or colour of the optic nerve, further tests will be recommended to diagnose glaucoma.
3-Pachymetry
This test is done to measure the thickness of the cornea. Some people’s corneas are so thick or thin that eye pressure readings get overestimated or underestimated by the tonometer. When the exact thickness of the cornea is known, eye pressure readings can be adjusted to get more accurate values.
4-Gonioscopy
This test is done to check whether or not the channel through which aqueous humour drains from the eye is open and wide enough. This can help determine the type of glaucoma one has as well as the best treatment option.
5-Perimetry
This test is done to assess the visual field of a suspected or confirmed glaucoma case. Your visual field is the extent you can see things on your sides while focusing on an object in front of you. Loss of vision in glaucoma starts from the side vision. So, the visual field test can determine whether vision loss due to glaucoma has started or not.
6-Optical coherence tomography
This is a test that uses the imaging technology to assess the optic nerve and other parts of the retina. It can detect early signs of glaucoma that are not yet visible to the human eye or do not show up on the visual field test result. This test is often recommended if you have risk factors for glaucoma or show signs of glaucoma that are not confirmed by the tests mentioned above. The results of this test can help the doctor make a definite diagnosis even at the very early stage of the disease.
Treatment
There are various treatment options for glaucoma. These include the use of medications, surgery, and drainage devices. These treatment options may be combined depending on your condition.
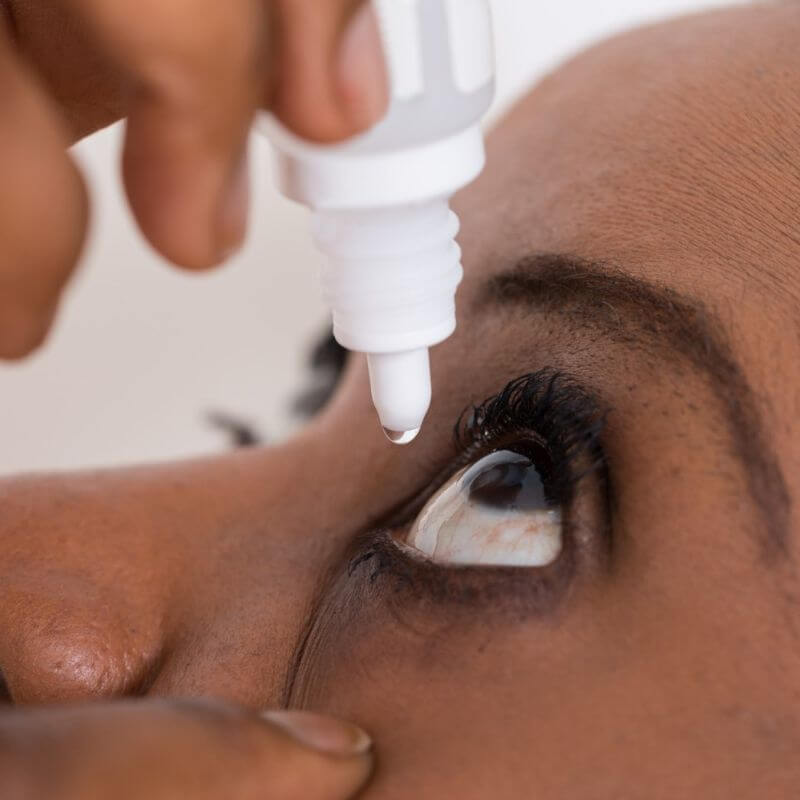
Medications
Glaucoma is frequently treated with eye drops. There are several classes of eye drops with varying mechanisms for reducing eye pressure. Some increase the drainage of aqueous humour, some reduce the production of aqueous humour while other combine both mechanisms to reduce eye pressure. On rare occasions, eye drops may be combined with tablets.
Surgery
Surgery is usually done for the treatment of angle-closure glaucoma or other types of glaucoma where medications do not lower the intraocular pressure. The common types of glaucoma surgery are laser surgery and conventional surgery. In laser surgery, known as trabeculoplasty, a laser beam is used to create a hole in the iris allowing more outflow of aqueous humour. The conventional glaucoma surgery called trabeculectomy involves the creation of a new channel through which aqueous humour can flow out.
Insertion of drainage devices
The use of drainage devices is usually the last option in glaucoma management. They are inserted into the eye under the conjunctiva with the tube positioned into the anterior chamber of the eye. They have been used to successfully lower eye pressure in cases where surgery failed.